How stress and anxiety can trigger IBS symptoms
Stress can trigger IBS symptoms because the brain and digestive system communicate through the gut-brain axis – the connection that links emotions, stress signals, and digestion. When the brain senses stress or anxiety, it can change how the gut moves, how sensitive it becomes, and how digestion functions.
Many people notice this connection in everyday life. Your stomach might tighten before a stressful meeting, a difficult conversation, or an important event. Symptoms like bloating, cramping, nausea, diarrhea, or constipation can appear quickly when the body is under pressure.
This connection is especially important in conditions known as gut-brain disorders – digestive conditions where communication between the brain and gut becomes disrupted. IBS (irritable bowel syndrome) is the most common of these disorders.
For people living with IBS, stress can act like an amplifier for digestive symptoms. When the nervous system is under strain, the gut can become more sensitive and digestive muscles may contract differently, making normal sensations in the intestines feel painful or uncomfortable.
Understanding this stress–digestion connection is often the first step toward managing symptoms more effectively.
In this guide, you will learn:
• what IBS is and how stress influences symptoms
• why IBS flare-ups often happen during stressful periods
• how the gut-brain connection links emotions and digestion
• evidence-based ways to calm stress-related digestive symptoms
What is IBS and why does stress make symptoms worse?
IBS (irritable bowel syndrome) is one of the most common gut-brain disorders, meaning symptoms are influenced by how the brain, nervous system, and digestive system communicate with each other.
People with IBS often experience abdominal pain, bloating, diarrhea, constipation, or unpredictable changes in bowel habits. Symptoms usually appear in cycles known as flare-ups, where digestion becomes more uncomfortable for a period of time before settling again.
Unlike digestive diseases that cause visible damage to the intestines, IBS affects how the digestive system functions. The nerves that control digestion can become more sensitive, meaning the gut may react more strongly to everyday triggers.
Stress is one of the most common of these triggers. Busy schedules, anxiety, illness, travel, and major life changes can activate the body’s stress response, making the digestive system more reactive and increasing the likelihood of symptom flare-ups.
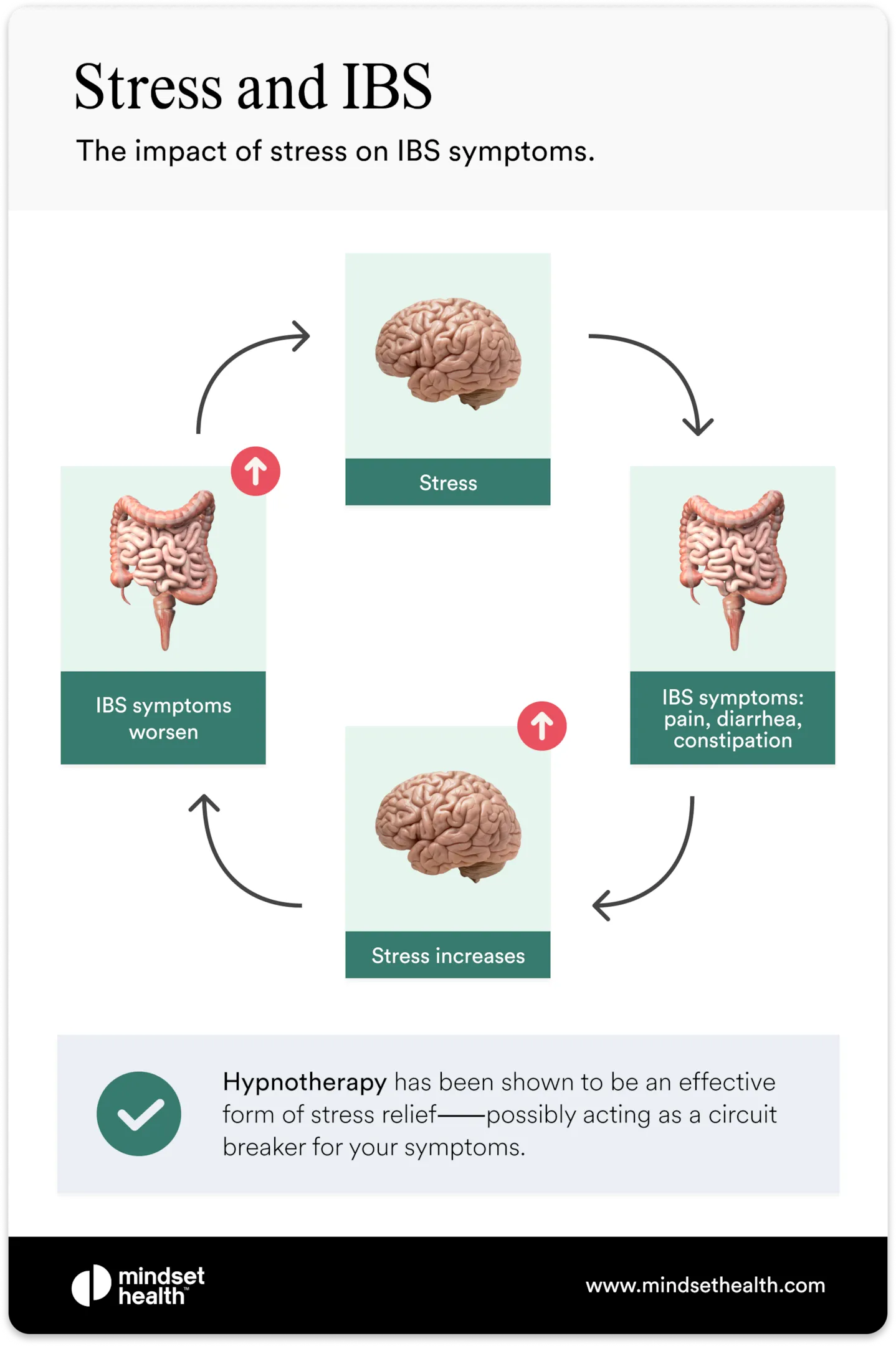
Common IBS symptoms and how stress can trigger flare-ups
IBS symptoms vary from person to person, but they usually involve abdominal discomfort and changes in bowel habits. Symptoms often come and go, with periods of relative calm followed by flare-ups.
Common IBS symptoms include:
• abdominal pain or cramping
• bloating or visible stomach swelling
• excess gas
• diarrhea or loose stools
• constipation
• alternating diarrhea and constipation
• a feeling of incomplete bowel movements
For many people, these symptoms become more noticeable during stressful periods. When the body experiences stress, the nervous system can change how the digestive system moves and how strongly sensations in the gut are felt.
This is why many people notice symptoms worsening during deadlines, exams, travel, illness, or major life events. For people living with gut-brain disorders like IBS, stress does not just affect mood – it can directly influence how the digestive system behaves.
What is the gut-brain connection? Why stress affects digestion
The reason stress can influence digestion so strongly is the gut-brain connection, also known as the gut-brain axis. This is the communication system that links your brain and digestive system, allowing them to constantly send signals back and forth.
Researchers at Monash University – the institution that developed the low FODMAP diet and leads global research on IBS – explain that this two-way communication means emotional stress can influence how the digestive system functions, while ongoing gut symptoms can also affect mood and anxiety. In other words, the brain and gut are always influencing each other.1
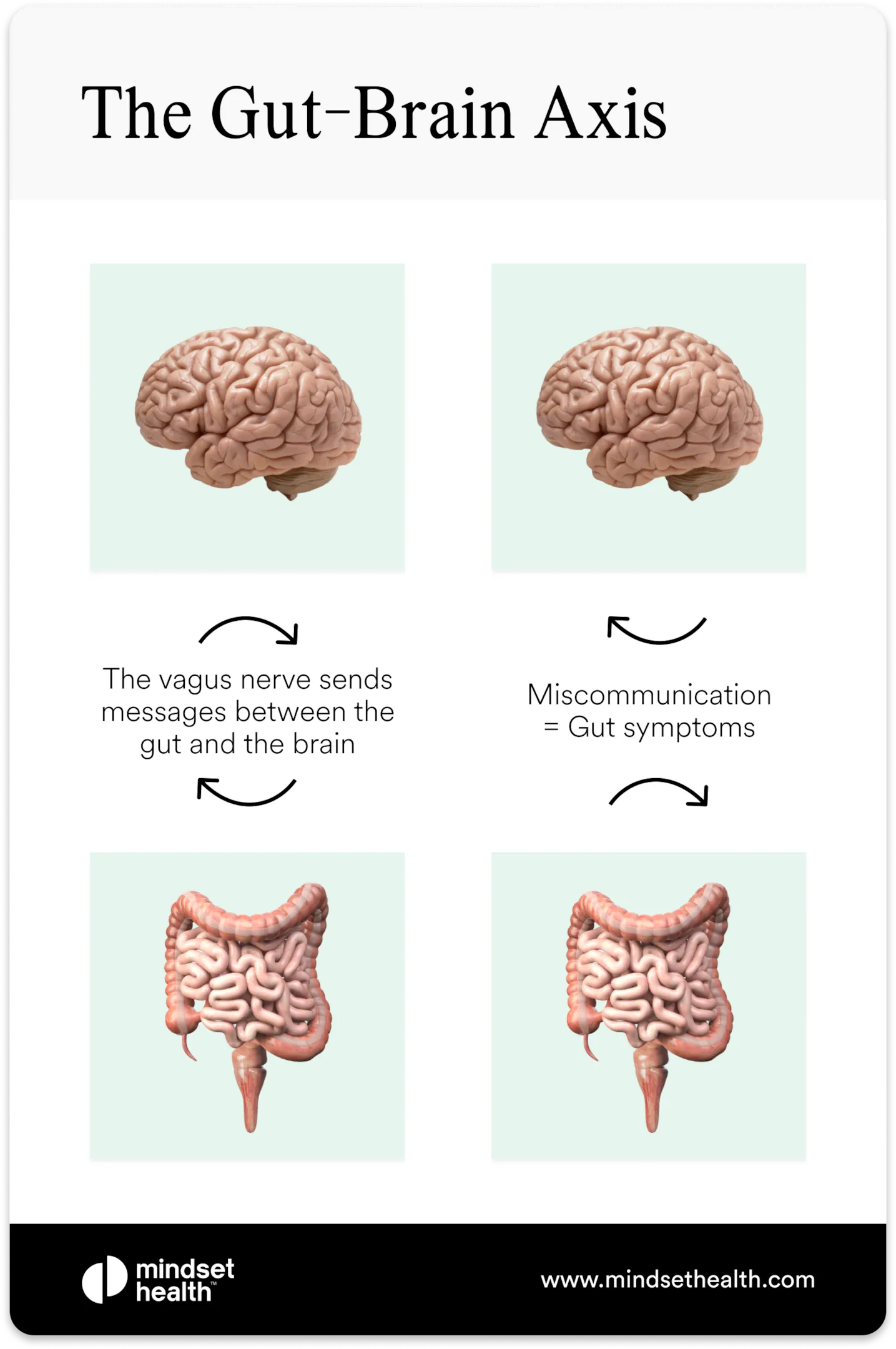
You may have already experienced this connection in everyday life. Many people notice their stomach tightening before a stressful event, feeling nauseous during anxiety, or needing the bathroom urgently when they are nervous. These reactions happen because the brain and gut are closely linked through the nervous system.
The gut actually contains millions of nerve cells that communicate directly with the brain through pathways such as the vagus nerve. Because of this constant signaling, emotional stress can quickly influence how the digestive system moves, how sensitive it feels, and how strongly sensations are perceived.
Gastroenterologist Dr. Mark Salvatore, pediatric GI specialist at Massachusetts General Hospital and Harvard Medical School, notes that this connection is reflected in the body’s chemistry as well. “About 95% of the body’s serotonin is actually located in the gastrointestinal tract, not the brain,” he explains, highlighting how closely the nervous system and digestive system are linked.
What is the fight or flight response?
When the brain detects stress, it activates the body’s fight-or-flight response. This response prepares the body to deal with a threat, but it temporarily shifts energy away from digestion.
As a result:
• digestion may speed up or slow down
• gut muscles may contract differently
• the digestive system may become more sensitive to normal sensations
For people living with IBS and other gut-brain disorders, this stress response can act like an amplifier. Sensations that might normally feel mild can become uncomfortable or painful, and digestive symptoms may flare more easily during stressful periods.
Understanding this connection can be reassuring. It does not mean symptoms are “in your head.” Instead, it reflects the very real biological relationship between the nervous system and the digestive system – and why approaches that support both the mind and gut can help improve symptoms.
Brain-gut therapy, tailored to you
Fix the miscommunication between your back and brain
Overcome life's challenges
Take control of hot flashes and night sweats
Quit smoking in 3 weeks
How stress affects the body and digestion
Stress is the body’s natural response to pressure, challenge, or uncertainty. When the brain detects stress, it releases hormones such as cortisol and adrenaline that prepare the body to react quickly.
Gastroenterologist Dr Jeffrey Nathanson of Comprehensive Gastrointestinal Health says this connection often shows up in patients who otherwise appear calm and high-functioning. “Often I’ll see a lot of very high-achieving individuals – successful in their personal and professional lives – who don’t register stress or anxiety in any other way except through their gastrointestinal symptoms,” he explains.
In the short term, this stress response can increase focus and alertness. But when stress occurs frequently or lasts for long periods, it can begin to influence how the digestive system functions.
Over time, repeated stress activation can:
• increase gut sensitivity
• disrupt normal digestive movement
• change pain signaling between the gut and brain
• alter hormone and immune activity
For people living with IBS and other gut-brain disorders, this ongoing stress response can make the digestive system more reactive and symptoms more likely to flare.
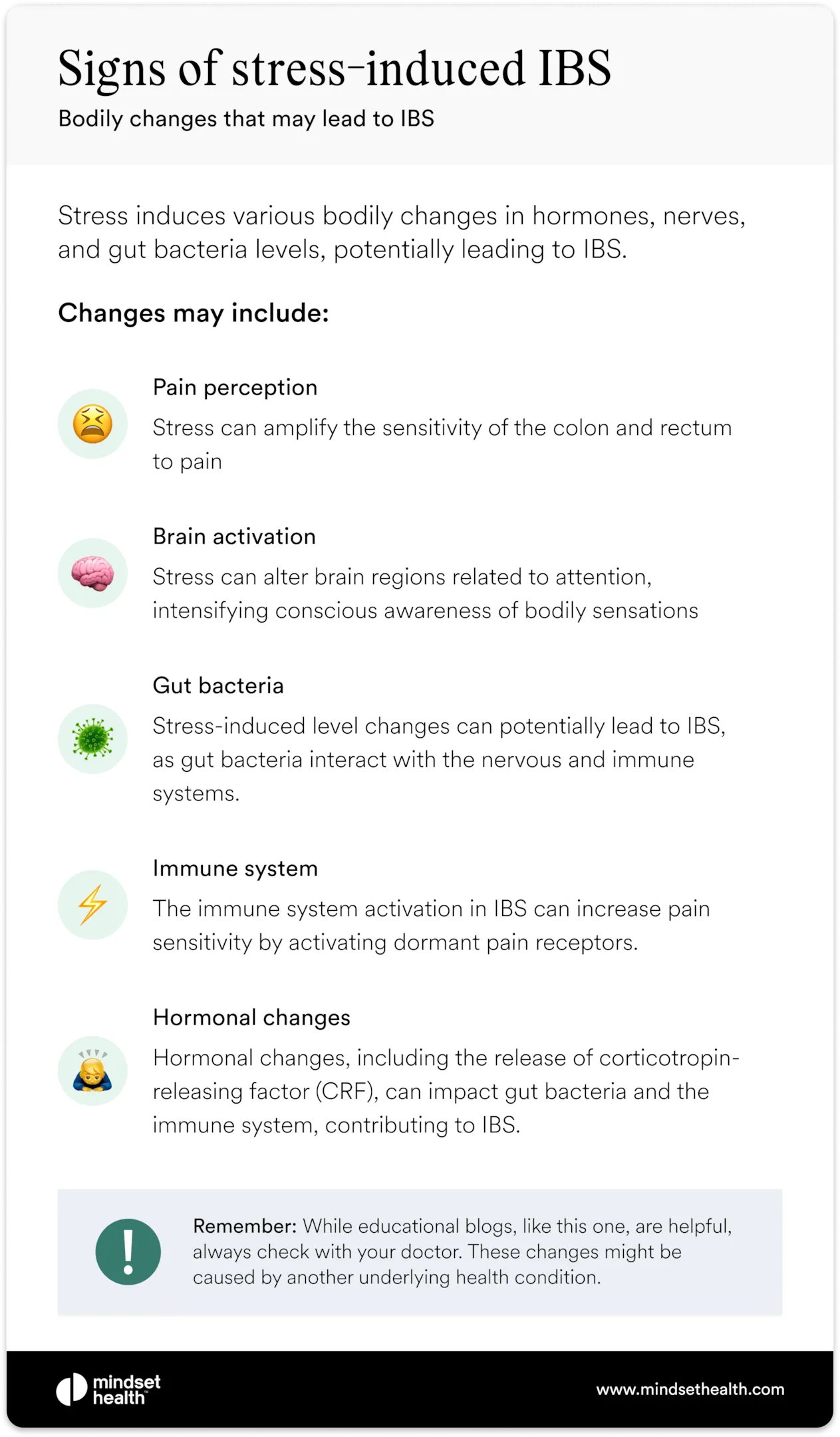
What research shows about stress and IBS
Research supports what many people with IBS already notice: stress can make symptoms worse. In a 16-month study following people with IBS, those experiencing higher levels of chronic life stress were much more likely to have ongoing or worsening symptoms.2
Other clinical studies show that people with IBS often have increased sensitivity in the digestive tract, known as visceral hypersensitivity.3 4 This means the nerves in the gut react more strongly to normal digestive activity, especially during stressful situations.
Other clinical studies show that people with IBS often experience greater sensitivity in the digestive tract during stressful situations. This heightened sensitivity is known as visceral hypersensitivity, meaning the nerves in the gut respond more strongly to normal digestive activity.
Because of this increased sensitivity, stress can directly influence how the digestive system processes sensations, making symptoms such as pain, cramping, or bloating feel more intense.
For many people living with IBS, these findings confirm something they already notice in daily life – stressful periods often coincide with worsening digestive symptoms.
How chronic stress changes the gut
When stress becomes ongoing, it can influence several important processes within the digestive system.
Research shows chronic stress can:
• increase muscle contractions in the intestines, causing cramps and urgency
• slow digestion, which may contribute to constipation
• alter the balance of gut bacteria in the microbiome
• increase inflammation in the digestive system
• amplify pain signaling between the gut and brain
These changes can make the digestive system more sensitive and reactive over time, which is why IBS symptoms often become more noticeable during prolonged stressful periods.
The role of trauma and emotional health in IBS
Emotional health and life experiences can also influence the gut-brain system.
Studies suggest that a significant number of people with IBS have experienced major life stressors or trauma. Events such as loss, long-term anxiety, emotional abuse, or other difficult experiences can keep the body’s stress response activated for longer periods.
Research also shows a strong connection between trauma and digestive disorders. GI Dr. Mark Salvatore notes that many people with gut-brain disorders have experienced significant life stress or trauma. Research supports this pattern – a systematic review found that about one in five people with gastrointestinal conditions experience post-traumatic stress disorder (PTSD).5
When the nervous system remains on high alert, digestive signals may feel stronger and symptoms may become more persistent.
Addressing emotional health does not mean symptoms are “in your head.” Instead, it reflects the close relationship between the nervous system and the digestive system.
Approaches that support emotional well-being and nervous system regulation can often play an important role in improving symptoms for people with gut-brain disorders.
Evidence-based ways to calm stress-related IBS symptoms
Because IBS is closely connected to the gut-brain system, treatments that support both the nervous system and digestion can be especially helpful.
Research supports several approaches that reduce symptoms by calming the gut-brain connection.
These include:
• gut-directed hypnotherapy, which uses guided relaxation to regulate communication between the brain and digestive system
• cognitive behavioral therapy (CBT), which helps shift thought patterns that increase anxiety and symptom anticipation
• mindfulness and relaxation techniques that reduce nervous system activation
• gentle movement such as yoga or walking to support digestion and stress regulation
These approaches help the nervous system return to a more balanced state, which can reduce the intensity and frequency of IBS symptoms.
Lifestyle habits that reduce stress-related IBS flare-ups
Alongside targeted therapies, everyday habits can help regulate the gut-brain system and reduce IBS flare-ups during stressful periods.
Helpful habits include:
• regular movement such as walking, stretching, or yoga to lower stress hormones and support gut motility
• consistent sleep routines that help regulate cortisol and nervous system balance
• regular meal timing to support stable digestion
• relaxation practices such as breathing exercises, meditation, or journaling that activate the body’s “rest and digest” state
• supportive social connection, which helps reduce stress and improve emotional resilience
Over time, supporting the nervous system through daily routines can help calm the gut-brain connection and make the digestive system less reactive to stress.
Frequently asked questions
What is the connection between stress and IBS?
Stress and IBS are connected through the gut-brain axis – the communication network between the brain and digestive system. When stress increases, it can change gut movement and sensitivity, triggering IBS symptoms.
Can anxiety cause stomach problems?
Yes, anxiety can affect digestion because the brain and gut communicate constantly. Stress signals can cause symptoms such as nausea, stomach pain, bloating, diarrhea, or constipation.
Why does stress upset my stomach?
Stress activates the body’s fight-or-flight response, which temporarily disrupts digestion. This can change how quickly food moves through the gut and make the digestive system more sensitive.
How do I calm stress-related IBS symptoms?
Approaches that regulate the nervous system can help, including gut-directed hypnotherapy, mindfulness, cognitive behavioral therapy, gentle movement, and stress management techniques.
Can managing stress improve IBS symptoms?
Yes. Many studies show that reducing stress and calming the gut-brain connection can help reduce IBS flare-ups and improve digestive comfort.