SIBO (Small Intestinal Bacterial Overgrowth) is a digestive condition where excessive bacteria accumulate in the small intestine, leading to gas production, bloating, abdominal discomfort, and changes in bowel habits.
If you have been told you have SIBO – or you suspect it based on your symptoms – you are not alone. Many people first encounter the term after months, sometimes years, of unexplained bloating, pain, or unpredictable digestion.
SIBO is more common than many realize – it affects anywhere from 2.5% to 22% of people and is frequently missed for years.¹ It is also significantly more common in people with IBS, with some studies suggesting up to one-third of IBS patients have abnormal breath tests consistent with SIBO.²
This guide explains what SIBO is, why it develops, how it is diagnosed, what treatments are supported by evidence, and why symptoms sometimes continue even after bacterial levels are reduced.
Understanding the full picture is often the first step toward meaningful, lasting relief.
What is SIBO?
SIBO stands for Small Intestinal Bacterial Overgrowth. It occurs when bacteria build up in the small intestine in higher numbers than normal, interfering with digestion and triggering symptoms such as bloating, gas, abdominal pain, and altered bowel habits.
Under healthy conditions, most gut bacteria live in the large intestine. The small intestine contains relatively few bacteria, so food can be digested and nutrients absorbed efficiently.
So if you have SIBO, it means bacteria are building up in a part of your gut that is meant to stay relatively low in bacteria – and that can interfere with digestion right from the start.
One of the main reasons this buildup happens is reduced movement through the small intestine. Between meals, the gut normally generates gentle cleaning waves that sweep leftover food particles and bacteria downward. If this movement slows – after an infection, during chronic stress, or due to certain medical conditions – bacteria are not cleared properly and begin to multiply.
As food enters the small intestine, the excess bacteria ferment carbohydrates earlier than they should. This premature fermentation produces hydrogen or methane gas. Gas stretches the intestinal walls, creating pressure, visible bloating, abdominal discomfort, and changes in bowel habits such as diarrhea or constipation.
In simple terms, SIBO is not just “too much bacteria” – it’s bacteria in the wrong place, interfering with digestion and producing excess gas that leads to bloating, discomfort, and changes in bowel habits.
What are the symptoms of SIBO?
The most common SIBO symptoms are:
- persistent bloating
- excess gas
- abdominal discomfort
- changes in bowel habits.
Bloating is often the most distressing feature. Many people notice their abdomen becomes progressively more distended throughout the day, especially after meals. The discomfort can range from mild pressure to sharp cramping.
Because SIBO alters how carbohydrates are fermented, symptoms frequently worsen after eating foods that are high in fermentable carbohydrates.
Some people also experience early fullness, nausea, fatigue, or brain fog.
In longer-standing cases, impaired nutrient absorption may contribute to low vitamin B12 or iron levels.
Because SIBO symptoms look so similar to IBS and other gut-brain disorders, it’s not always obvious what’s causing them. A careful evaluation helps clarify what’s really happening.
What causes SIBO?
SIBO develops when bacteria are able to remain and multiply in the small intestine instead of being cleared effectively.
The most common underlying driver is slowed intestinal movement. This can occur after food poisoning, which may damage the nerves that coordinate gut movement. It can also occur in conditions that affect nerve or muscle function in the digestive tract.
Other contributing factors include thyroid disorders, diabetes, structural changes in the intestine, prior abdominal surgery, and long-term acid suppression therapy.
Chronic stress also plays a role.
The gut and brain communicate continuously, and prolonged stress can slow digestive movement. Over time, this can create an environment where bacterial overgrowth is more likely to develop or recur.
In many cases, SIBO is not the original problem. It is the consequence of disrupted gut movement and altered gut-brain signaling.
Brain-gut therapy, tailored to you
Fix the miscommunication between your back and brain
Overcome life's challenges
Take control of hot flashes and night sweats
Quit smoking in 3 weeks
How is SIBO diagnosed?
SIBO is most commonly diagnosed using a hydrogen or methane breath test. This test measures gases produced when bacteria ferment a sugar solution.
After drinking lactulose or glucose, breath samples are collected over several hours. A rise in hydrogen or methane suggests bacterial overgrowth in the small intestine.
Breath testing has limitations. Results can vary depending on preparation, timing, and interpretation. False positives and false negatives occur. For this reason, diagnosis should be based on a combination of symptoms, risk factors, and test results rather than relying on a single measurement.3
In some cases, healthcare providers may also evaluate nutrient levels or investigate underlying conditions that could contribute to overgrowth.
What is the best treatment for SIBO?
The most commonly prescribed treatment for SIBO is rifaximin, a non-absorbed antibiotic that works locally in the gut to reduce bacterial overgrowth.4
Treatment usually lasts 10 to 14 days. In methane-associated cases, combination therapy may be used.
Dietary strategies such as a low FODMAP approach can reduce symptoms by limiting fermentable carbohydrates. However, diet alone does not eliminate overgrowth and is generally used as a symptom-management tool rather than a cure.
Long-term improvement often depends on addressing the underlying cause. Supporting intestinal movement, managing thyroid or metabolic conditions, and reducing chronic stress are often part of a comprehensive approach.
Why does SIBO often come back?
SIBO frequently recurs because treatment reduces bacterial levels but does not always correct the reason overgrowth developed in the first place.
One study found that approximately 44% of people experienced recurrence within nine months after antibiotic therapy.5
If intestinal movement remains impaired, bacteria can accumulate again. In some cases, symptoms persist even when bacterial levels have improved. This may reflect increased gut sensitivity or ongoing disruption in gut-brain communication.
Recurrence does not necessarily mean treatment failed. It often means the underlying factors affecting gut movement and gut-brain signaling still need to be addressed.
Is SIBO a gut-brain disorder?
SIBO itself is not formally classified as a disorder of gut-brain interaction. However, it is closely connected to gut-brain disorders such as IBS, and the overlap is clinically important.
Gut-brain disorders happen when the communication between the gut and the brain becomes disrupted. Your digestive system and nervous system are constantly sending signals back and forth to regulate movement, sensitivity, and comfort. When those signals become unbalanced or overly sensitive, digestion can slow, the gut can become more reactive, and normal sensations like stretching or gas can feel uncomfortable.
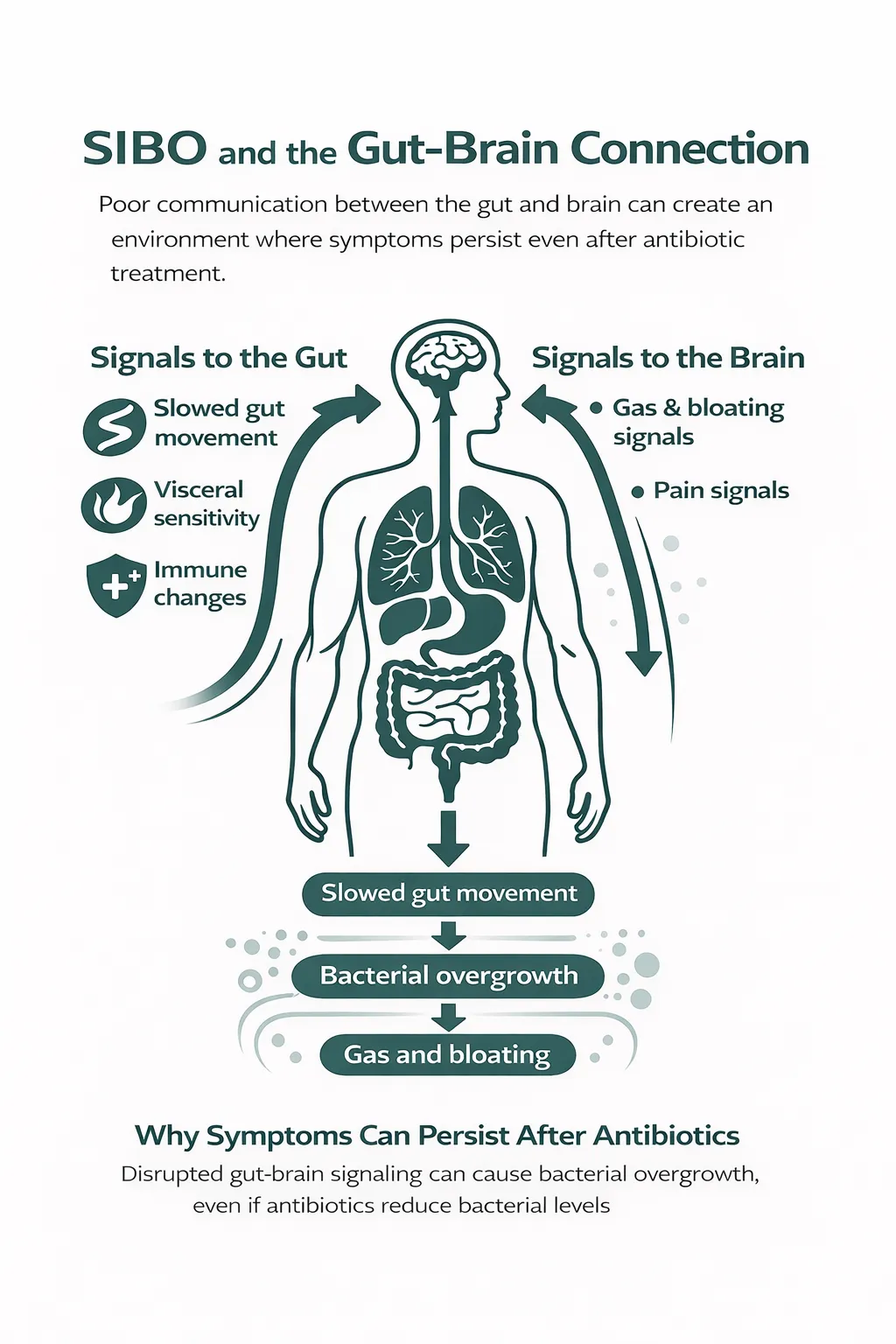
Many of the same factors that contribute to gut-brain disorders – including post-infectious nerve changes, chronic stress, and altered intestinal movement – also increase the risk of developing SIBO.
For many people, SIBO is part of a bigger picture. The same gut-brain disruptions that affect movement and sensitivity can also create conditions where bacterial overgrowth is more likely to develop.
This helps explain why bloating or pain can continue even after bacterial levels improve. In these situations, the overgrowth may be reduced, but increased gut sensitivity or ongoing nerve signaling changes are still driving symptoms.
Looking at SIBO through a gut-brain lens shifts the focus from bacteria alone to how the digestive system is functioning as a whole. For many people, lasting improvement means addressing both the bacterial overgrowth and the nervous system patterns that influence gut movement and sensitivity.
Is SIBO the same as IBS?
SIBO and IBS share many symptoms, but they are not the same condition.
SIBO is defined by bacterial overgrowth in the small intestine. IBS is classified as a disorder of gut-brain interaction (DGBI) and is diagnosed based on symptom patterns.
Some people with IBS have abnormal breath tests consistent with SIBO. Others do not.
Treating bacterial overgrowth does not always resolve IBS symptoms, particularly when altered gut sensitivity or gut-brain signaling remains active.
The overlap between SIBO and IBS helps explain why digestive symptoms can persist even after antibiotic treatment.
Can SIBO cause long-term complications?
In more severe or prolonged cases, SIBO can interfere with nutrient absorption.
Low vitamin B12, iron deficiency, fatigue, and unintended weight loss may occur if overgrowth significantly disrupts digestion. These complications are not typical in mild cases but should be evaluated if symptoms are persistent or worsening.
When should you see a doctor about SIBO symptoms?
Medical evaluation is important if you experience unexplained weight loss, blood in the stool, persistent vomiting, fever, severe abdominal pain, or symptoms that wake you from sleep.
These features are not typical of uncomplicated SIBO and require prompt assessment to rule out other conditions.
Frequently asked questions
Does SIBO go away on its own?
Mild cases may improve if digestive movement normalizes, but most persistent cases require targeted treatment. Without addressing underlying factors, symptoms often continue or recur.
Does stress make SIBO worse?
Chronic stress can slow digestive movement and increase symptom sensitivity. While stress alone does not directly create bacterial overgrowth, it can contribute to recurrence and ongoing discomfort.
Are probiotics helpful for SIBO?
Research on probiotics for SIBO shows mixed results.5 Some strains may help certain people, while others can worsen bloating during active overgrowth. Because responses vary, probiotic use should be individualized and discussed with a healthcare provider.
How long does recovery from SIBO take?
Some people notice improvement within weeks of treatment. Others require additional time to address underlying movement issues or gut-brain factors before symptoms stabilize.







