A gut-brain disorder is a condition where the communication system between the gut and the brain becomes disrupted – causing real, ongoing symptoms like pain, bloating, diarrhea, constipation, and nausea, even when scans and blood tests show no structural damage.
Living with symptoms like these – especially without a clear explanation – can be exhausting and confusing.
Questions like "has something been missed?" or "why do I feel this bad if my tests are normal?" are incredibly common.
What's important to understand is that a clear test result doesn't mean nothing is wrong – it means no structural damage was found.
This guide explains what gut-brain disorders are, why they cause the symptoms they do, and why they are more common and more manageable than most people realize.
What is a gut-brain disorder?
Your gut and your brain are in constant communication – exchanging signals through nerves, hormones, and chemical messengers that regulate digestion and interpret what the gut is sensing.¹
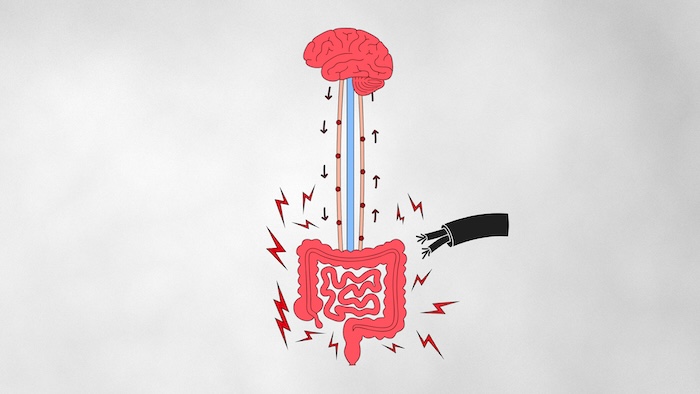
One of the main pathways in this system is the vagus nerve – a vast communication network running between the gut and the brain that helps coordinate everything from digestion to how strongly sensations are felt.

A disorder of gut-brain interaction – or DGBI – is what happens when this system becomes disrupted or hypersensitive. Symptoms aren't caused by visible damage or disease. Instead, they're driven by changes in how gut signals are sent, amplified, and interpreted by the nervous system.
To see how this works visually, the short video below walks through the role of the vagus nerve in gut-brain disorders – and why it matters for understanding your symptoms.
Types of gut-brain disorders
Gut-brain disorders cover a wide range of digestive conditions.
The most common include:
- Irritable bowel syndrome (IBS)
- Functional dyspepsia
- Functional constipation
- Functional diarrhea
- Rumination syndrome
- Reflux hypersensitivity
These conditions can look very different on the surface, but they share a common underlying feature – altered gut-brain communication. They are also far more common than most people realize, affecting millions of people worldwide.
While conditions like GERD (Gastroesophageal Reflux Disease), IBD (Inflammatory Bowel Disease), and SIBO (Small Intestinal Bacterial Overgrowth) are not classified as gut-brain disorders, they frequently overlap with them – and gut-brain sensitivity can significantly influence how symptoms are experienced in all three.
If you've been diagnosed with one of these conditions, your symptoms fit a well-recognized medical pattern – and you are not alone.
For a one-page visual summary of how gut-brain disorders develop and why symptoms feel the way they do, download the fact sheet below.

How does the gut-brain connection cause symptoms?
Think of the gut-brain connection like a volume dial.
Everyone has a built-in system that controls how strongly sensations from the gut are felt. Most of the time, that dial is set low – digestion happens quietly in the background, and you barely notice it.
In some people, the sensory nerves in and around the gut become more sensitive. This means everyday digestive activity – such as movement, gas, fullness, or bowel contractions – can feel louder or more intense than usual, even though the gut itself isn't damaged.

What is visceral hypersensitivity?
Visceral hypersensitivity is the term used to describe this increased nerve reactivity in the gut.² When signals from the gut become amplified, the brain may interpret them as a problem – even when nothing harmful is happening.
In response, it can send stronger signals back to the gut, further amplifying symptoms like:
- Discomfort or pain
- Urgency
- Bowel changes
- Bloating or distension
- Nausea or reflux symptoms
Once this volume is turned up, the pattern tends to reinforce itself – meaning symptoms can be triggered more easily over time, even by completely normal digestive processes.
Brain-gut therapy, tailored to you
Fix the miscommunication between your back and brain
Overcome life's challenges
Take control of hot flashes and night sweats
Quit smoking in 3 weeks
Why do my tests keep coming back normal?
Many people assume that persistent, painful symptoms must come from visible disease. It's a reasonable assumption – and it's exactly why healthcare providers take symptoms seriously and order tests.
But not all medically significant conditions show up on imaging, scopes, or blood work.
Gut-brain disorders are diagnosed based on symptom patterns and how the nervous system is functioning – not structural damage.
A normal test result doesn't mean nothing is happening. It means no dangerous structural condition – such as inflammatory bowel disease, ulcers, or cancer – was found. That's an important distinction.
Once structural disease has been ruled out, the focus shifts toward understanding what type of gut-brain dysfunction may be driving symptoms. For many people, that shift can feel unsettling at first – especially when symptoms continue, change, or flare unpredictably.
It's completely understandable to want more testing. A clear scan can bring temporary relief, but that reassurance often fades when symptoms return. Over time this can create a cycle – ongoing symptoms lead to repeated investigations, which reinforce the feeling that a hidden cause still hasn't been found.
As gastroenterology nurse practitioner Amy Stewart of Capital Digestive Care tells her patients, "Gut-brain disorders are real, and we can do real things about it. You don't have to live like this, and we can improve your quality of life."
Once structural disease has been ruled out, the most helpful next question becomes: what is driving this symptom pattern, and why is the gut-brain system staying on high alert?
Does a gut-brain diagnosis mean it's all in my head?
If tests have ruled out disease, it can still be hard to hear terms like "hypersensitivity," "nervous system," or "stress response." Many people worry it means their healthcare provider believes their symptoms are psychological.
But a gut-brain explanation is a physiological explanation. It describes how the nervous system communicates with the gut and how those signals can become amplified. Symptoms are never "all in your head" – they have a real, measurable biological basis.
As Amy Stewart explains, this amplification can quickly become a self-reinforcing cycle:
"The gut-brain connection is well defined in the literature. Your brain sends physiological signals to your gut that there is a problem, and gets it all riled up. Then you don't feel good and you worry about these symptoms, asking yourself 'Is there something really very seriously wrong? Did we miss something? Am I going to be able to get out of the house and get to work on time without stopping to get to a bathroom?' Of course, you're worried about these symptoms, as who wouldn't be?"
This kind of amplified back-and-forth signaling between the gut and brain is a recognized mechanism in disorders of gut-brain interaction.³ It helps explain why symptoms can feel intense, disruptive, and frightening – even when no structural disease is found.
Why do gut-brain disorder symptoms come and go?
If you have a gut-brain disorder, you've likely noticed your symptoms fluctuating – some days feel manageable, while others feel overwhelming.
That unpredictability is one of the most frustrating and confusing aspects of these conditions, and it's completely understandable to wonder why.
Because the gut-brain system is responsive rather than static, symptoms can be influenced by many factors – often at the same time:
- Digestion itself
- Sleep disruption
- Prior flare-ups
- Hormonal changes
- Illness or antibiotics
- Heightened nervous system alertness
In many cases, symptoms aren't tied to a single trigger. Instead, they reflect a system that has become more reactive over time – responding more strongly to everyday inputs that wouldn't previously have caused a problem.
Can diet fix a gut-brain disorder?
Many people with a gut-brain disorder assume their symptoms must be caused by something they ate – especially when flare-ups seem connected to meals. Food can absolutely act as a trigger, but it is not usually the underlying cause.
Foods high in FODMAPs – like onions, apples, and wheat – naturally create pressure, gas, and movement in the gut. This happens in everyone. The difference in gut-brain disorders is that the nerves in the gut are more sensitive, so those same normal processes can feel louder, more urgent, or more painful than they should.
This is why everyday foods can sometimes lead to outsized symptoms – not because the food itself is harmful, but because it is passing through a sensitized system.
Dietary changes can help reduce symptoms for some people by lowering the digestive load the gut has to process. But they don't retrain the gut-brain signaling system itself.⁴ This is why symptoms can return, shift, or flare unpredictably over time – even when someone feels they are doing everything right.
You are not imagining this
Gut-brain disorders are real, medically recognized conditions affecting millions of people worldwide.
If you have felt dismissed, confused, or unsure whether your symptoms "count" – that experience is more common than you might think.
There is a clear physiological explanation for what you are experiencing. The gut-brain system is disrupted, not damaged – and that distinction matters, because it means there is a path forward.
Watch this vdeo to better understand gut-brain disorders.
Frequently asked questions
What is a gut-brain disorder?
A gut-brain disorder like IBS is a condition where the communication system between the gut and the brain becomes disrupted – causing real symptoms like pain, bloating, diarrhea, constipation, and nausea, even when scans and blood tests show no structural damage. They are medically recognized and far more common than most people realize.⁵
Why do my tests keep coming back normal if I have real symptoms?
Because gut-brain disorders don't cause structural damage – they cause a change in how the nervous system processes signals. Normal test results mean no dangerous structural condition was found. They don't mean nothing is wrong, and they don't mean your symptoms aren't real.
What is visceral hypersensitivity?
Visceral hypersensitivity is increased sensitivity of the nerves in the gut, making normal digestive activity – stretching, gas, and bowel contractions – feel more intense or painful than it should. It is a core feature of gut-brain disorders and explains why symptoms can be severe even when tests are normal.
Is a gut-brain disorder all in my head?
No. A gut-brain explanation is a physiological explanation. It describes how the nervous system communicates with the gut and how those signals can become amplified. Symptoms have a real, measurable biological basis – they are never purely psychological.
Why do gut-brain disorder symptoms come and go?
Because the gut-brain system is responsive rather than static. Symptoms can be influenced by digestion, sleep, stress, hormonal changes, illness, and nervous system alertness – often at the same time. This is why symptoms fluctuate and are not always tied to a single trigger.
Can diet fix a gut-brain disorder?
Dietary changes can reduce symptoms by lowering the digestive load the gut has to process – but they don't retrain the gut-brain signaling system itself. This is why symptoms often return or shift even when someone is managing their diet carefully. Addressing the underlying sensitivity produces better long-term results.